Pain Conditions We Treat
At Padda Institute, our pain management specialists & pain specialist doctors provide you the guidance and treatments tailored to your needs. We are best at what we do; we diagnose and evaluate to determine your best treatment plan, so that you can experience chronic pain relief like never before.
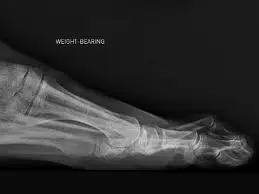
Facet Joint Radiofrequency (Rf)
A patient with primary facet pain, proven with either one or more blocks, may be a candidate for a facet rhizotomy using radiofrequency (RF)..
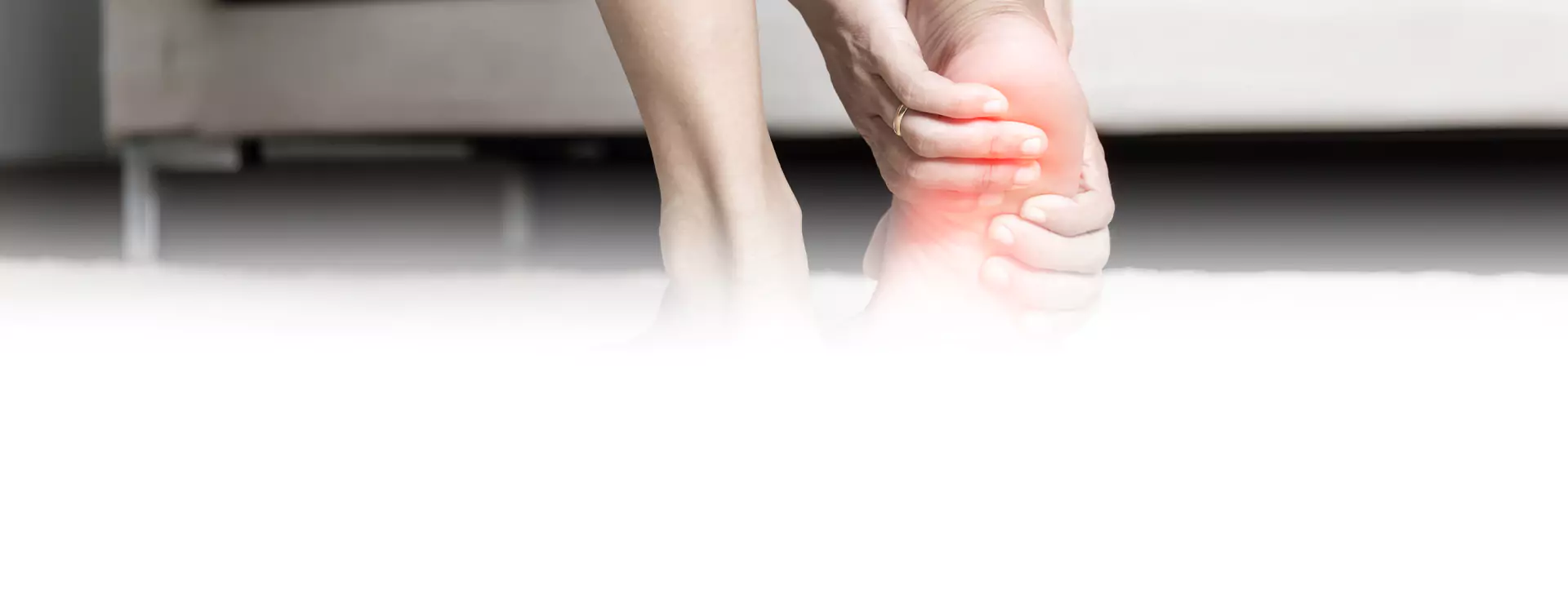
Diabetes And Neuropathy
Diabetic Peripheral Neuropathy (DPN) is the most common complication of diabetes, and often presents as a distal, symmetric..
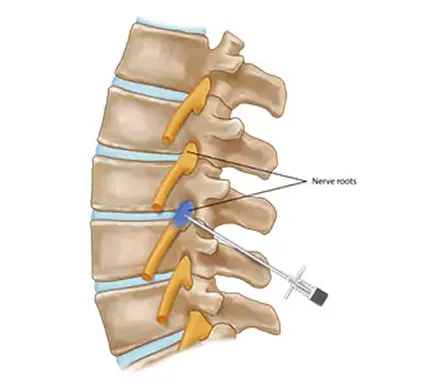
Selective Nerve Root Block
Nerve roots exit your spinal cord and form nerves that travel into your arms or legs. These nerves allow you to move your arms, chest wall, and..