Pain Conditions We Treat
At Padda Institute, our pain management specialists & pain specialist doctors provide you the guidance and treatments tailored to your needs. We are best at what we do; we diagnose and evaluate to determine your best treatment plan, so that you can experience chronic pain relief like never before.
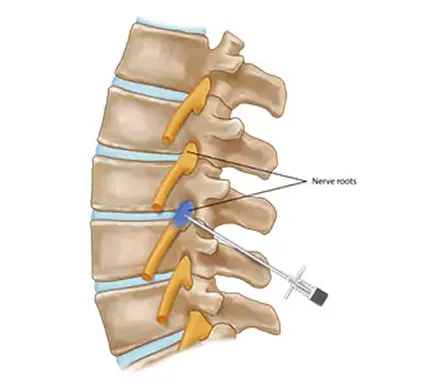
Selective Nerve Root Block
Nerve roots exit your spinal cord and form nerves that travel into your arms or legs. These nerves allow you to move your arms, chest wall, and..
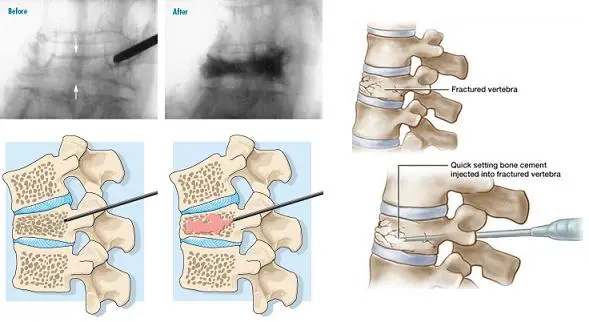
Discogram
The disks are soft, cushion-like pads which separate the hard vertebral bones of your spine. A disk may be painful when it bulges, herniates..
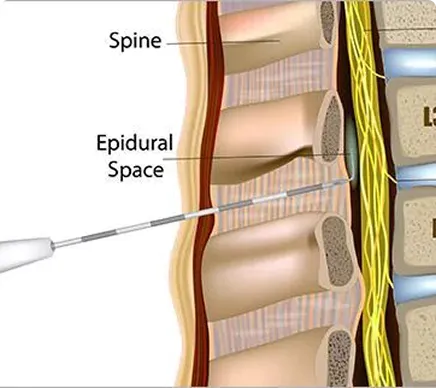
Epidural Steroid Injection (ESI)
Back pain affects nearly everyone at some point in their adult life. Often times the exact cause of pain is not readily apparent, as there are many..