Summary: Chronic persistent pains are pretty common. There are no signs of physical illness in many cases, and lab tests fail to show any significant changes. Most of these conditions are diagnosed as fibromyalgia, chronic fatigue syndrome, and psychogenic pains. Doctors would often find it challenging to manage these pains. They might use NSAIDs, opioids, antidepressants, antiseizure, and other drugs to reduce pain. However, treatment with these therapies is less than satisfactory. Researchers found that the use of corticosteroids like prednisolone help in some of the cases, and it may help relieve pain quite quickly. However, the success of prednisolone therapy in some patients points to immune dysregulation. Researchers have now found that autoimmune reactions cause many such pains. Many such individuals have high levels of leucine-rich glioma-inactivated 1 (LGI1) and contactin-associated protein-like 2 (CASPR2) antibodies.
Pain is quite an unpleasant feeling, often signaling that something is wrong with the body, but not always. Everyone has experienced this unpleasant sensation in their life. Some times source of pain is quite clear, like trauma, but sometimes unclear.
Pain is part of the so-called nociception system. It helps the body keep track of all the external and internal changes, from temperature to injury. However, the sensation of pain is quite complicated as it results from processing by higher brain centers.
Generally, the so-called nociceptive pain is pretty simple to understand. It is a pain caused by the stimulation of pain receptors due to external irritation. It helps a person escape the source of pain and damage to the body.
However, it is far more challenging to understand chronic persistent pains. In these pains, there is something wrong with the pain circuit. This damage or changes may have occurred at any place, in peripheral pain receptors, in the nerves, in the pathway in the spinal cord, and even in the brain. This kind of pain often requires specialized approaches for relief, such as interventional pain management in St. Louis, to help patients manage and alleviate these persistent pain sensations.
Further, it appears that many people are living with difficult-to-explain pains. In these individuals, lab tests do not show any changes, and quite often, other symptoms except pain are absent.
Just take an example of fibromyalgia, chronic fatigue syndrome, or prolonged body aches after some illness. It takes quite a long to diagnose these conditions, as everything appears to be fine with the body. These conditions often occur after some illness, but a person continues to experience body pains even after recovery. In many cases, body aches become a severe problem in the absence of any visible illness.
Researchers are still not fully clear why such chronic, persistent body aches occur. One of the theories is that these pains happen due to some changes in the brain centers that process pain. These brain centers become hypersensitive to pain. Thus, the brain starts processing even minor changes in the environment as pain1.
Book An Appointment With Us Today!
Doctors have also struggled to manage such generalized painful syndromes. They might give pain killers, and even antidepressants, antiseizure drugs, and opioids. Even worst that in many conditions, these potent drugs fail to help adequately.
However, researchers knew that they were missing something. Just take an example of the case of 66 years old patient. She presented with severe pain in both feet for the last 18 months, and later pain spread to influence thighs, buttocks, arms, and even torso. Doctors diagnosed it as fibromyalgia or psychogenic pains and treated it with pain killers and antidepressants, but the treatment did not help much. However, adding high dose prednisolone provided almost instant relief. Moreover, pains returned on the discontinuation of prednisolone2.
Prednisolone is a drug that suppresses inflammation and immunity. It is often used to treat autoimmune conditions. Its effectiveness in some patients living with chronic and persistent pain prompted them to look into the autoimmune mechanism of pain.
Figure 1 The role of LGI1 and CASPR2 antibodies in chronic persistent pains2
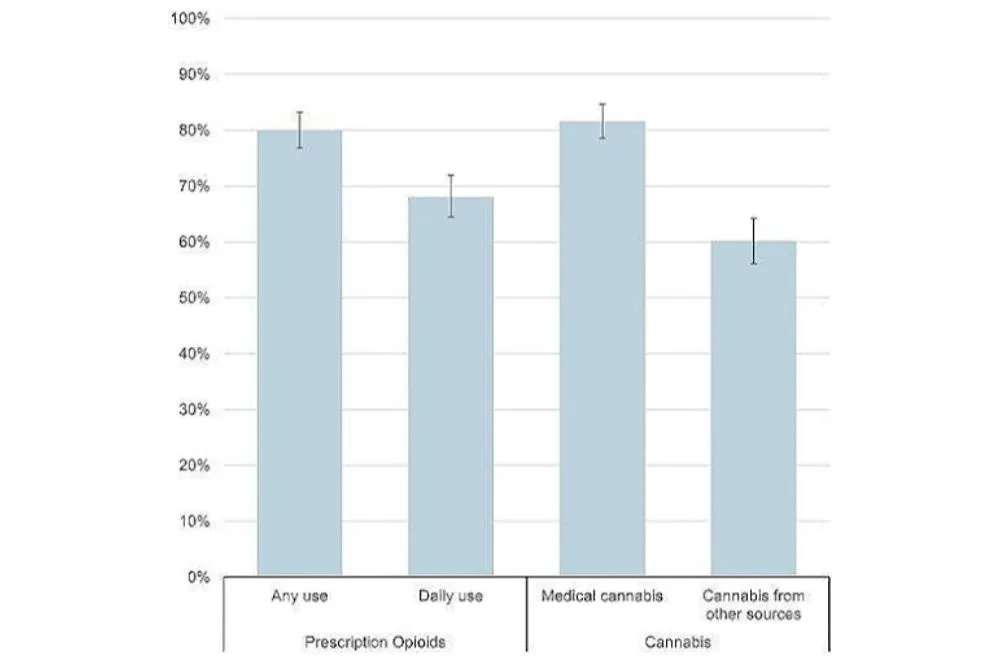
In a large group of 147 patients presenting with chronic and persistent pain, a kind of pains often reported by those living with fibromyalgia, researchers found that those who had leucine-rich glioma-inactivated 1 (LGI1) and contactin-associated protein-like 2 (CASPR2) antibodies were more likely to experience such pains2.
Further, researchers found that those with LGI1 antibodies responded much better to immunotherapy than those with CASPR2 antibodies. It means that these antibodies cause pain in different ways.
These findings are significant because they may help treat patients diagnosed with fibromyalgia or psychogenic pains. As of now, treatment of these painful sicknesses is not very effective. It is because doctors had no understanding of the underlying mechanism. Thus, this research furthers the understanding of pain and the therapeutic approach to certain types of pain syndromes.
References
- Animals NRC (US) C on R and A of P in L. Mechanisms of Pain. National Academies Press (US); 2009. Accessed October 17, 2021. https://www.ncbi.nlm.nih.gov/books/NBK32659/
- Ramanathan S, Tseng M, Davies AJ, et al. Leucine-Rich Glioma-Inactivated 1 versus Contactin-Associated Protein-like 2 Antibody Neuropathic Pain: Clinical and Biological Comparisons. Annals of Neurology. 2021;90(4):683-690. doi:10.1002/ana.26189
Gurpreet Singh Padda , MD, MBA, MHP